If your prostate cancer comes back
What is recurrent prostate cancer?
Recurrent prostate cancer is when your cancer comes back after you’ve had a treatment that aimed to cure it. It's sometimes called prostate cancer recurrence or prostate cancer relapse.
Treatments that you might have had include:
- surgery (radical prostatectomy)
- external beam radiotherapy (EBRT)
- permanent seed brachytherapy
- high dose-rate brachytherapy
- high intensity focused ultrasound (HIFU)
- cryotherapy
All these treatments aim to get rid of the prostate cancer. But sometimes not all the cancer is successfully treated, or the cancer may have been more advanced than first thought.
Finding out your cancer has returned
It can be very difficult to learn that your cancer has come back. All the thoughts and feelings you had when you were first diagnosed can come back again and they may be even stronger than before.
It's normal to feel shocked, angry, frustrated, disappointed, worried or sad. All these are very normal ways to feel. Things can get easier over time but some of these feelings may stay with you. Lots of men find it helpful to talk to someone about their feelings. This might be a friend or family member or someone who is trained to listen, like a counsellor or your doctor or nurse. You can also talk to our Specialist Nurses or someone who’s been there through our one-to-one support service or online community.
How do I know if my prostate cancer has come back?
Everyone’s prostate cancer journey is different, and it can take many months or even years before there is any sign that your prostate cancer has come back. Your doctors and nurses will have monitored you after your first treatment to check for any signs that the cancer has come back.
Usually the first sign that your cancer is starting to return is a continuous rise in the level of prostate specific antigen (PSA) in your blood. The PSA test is a very effective way of checking how successful your treatment has been. It can't show for certain if prostate cancer has come back, or where it might be. But it can be a useful sign that the cancer may have come back. The exact change in PSA level that suggests your cancer has come back depends on which treatment you had. Read more about PSA levels after different treatments.
Your doctor may do other tests to check if, and where, your cancer has come back. These may include a CT (computer tomography), MRI (magnetic resonance imaging), bone, or PET (positron emission tomography) scan. Read more about follow-up after treatment for prostate cancer.
What symptoms should I look out for?
If your cancer does come back, the first sign is likely to be a rise in your PSA level, rather than any symptoms.
However, it’s important to let your doctor or nurse know if you do get any new symptoms or side effects, or are worried that your cancer might have come back. Advanced prostate cancer (cancer that has spread from the prostate to other parts of the body) can cause symptoms, such as extreme tiredness (fatigue), bone pain and problems urinating. Physical problems will often be side effects of treatment rather than a sign that your cancer has come back.
Your doctor or nurse can help find out what might be causing your symptoms and help you manage any side effects. They can also look at your PSA level to see whether or not your cancer might have come back.
Why has my cancer come back?
It’s not always completely clear why prostate cancer comes back, but there are two main possible reasons.
- Not all of the cancer cells in your prostate were treated during your first treatment. Small groups of cells might have been left behind. Over time, these may have grown large enough to be picked up by tests or to cause symptoms.
- The cancer was more advanced than your doctor originally thought. Tests or scans you had when you were diagnosed might have missed small clusters of cancer cells outside your prostate, for example in your lymph nodes or bones (see the diagram below). Your first treatment would not have been aimed at these cells. Over time, these cells may have grown large enough to be picked up by tests or to cause symptoms.
When you were diagnosed, your doctor would not have been able to tell you whether or not your cancer would come back. But they may have said how likely it was. Read more about your chance of cancer coming back.
Where could my prostate cancer come back?
Your prostate cancer can have come back in one or more areas. It could be:
- in your prostate, if it hasn’t been removed by surgery
- in the area around where your prostate used to be (the prostate bed) if the prostate has been removed by surgery
- in the area just outside your prostate
- in other parts of your body.
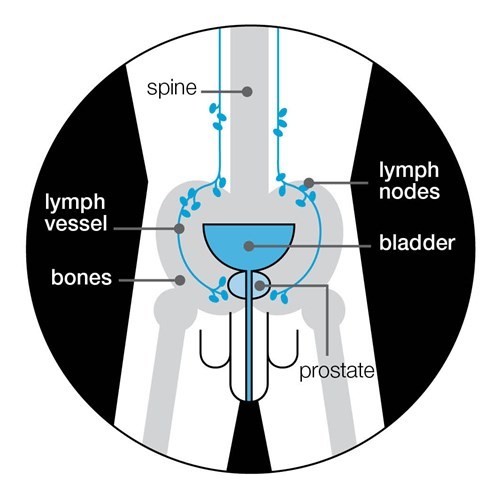
Prostate cancer can spread to any part of the body but it most commonly spreads to the bones and lymph nodes.
Prostate cancer that has spread to other parts of the body is known as advanced prostate cancer.
Sometimes it’s not clear where the cancer is. Some men may have a rise in their PSA level but the cancer may not show up on other tests, at least at first. This is quite common and your doctor will discuss treatment options with you.
What treatments are there for recurrent prostate cancer?
Treatments for recurrent prostate cancer are called second-line or salvage treatments. Many of the treatments used to treat prostate cancer when it’s first diagnosed can also be used as second-line treatments.
Making a decision about treatment
Your doctor might offer you one treatment, or a choice of treatments for recurrent prostate cancer. You may also be able to have your cancer monitored rather than treated straight away (see below). Or you might decide you don't want more treatment, other than treatment to help manage any symptoms you might get.
All treatments have advantages, disadvantages and side effects. Everyone is different and some side effects might be a problem for one man but not for another. It’s important to discuss your options with your doctor before deciding on a treatment. You could also talk through your options with your partner, family or friends, or speak to our Specialist Nurses.
What second-line treatments are there?
There are two main types of treatments – those that aim to get rid of the cancer (curative treatments) and those that aim to delay the cancer growing but won’t get rid of it.
Treatments aiming to get rid of the cancer
- External beam radiotherapy uses high-energy X-ray beams to destroy cancer cells. You might have it with or without hormone therapy.
- Permanent seed brachytherapy involves implanting tiny radioactive seeds into your prostate.
- High dose-rate brachytherapy involves inserting thin tubes into the prostate. A source of radiation is passed down the tubes into the prostate for a few minutes. The tubes are then taken out.
- Surgery (radical prostatectomy) removes your prostate and the cancer inside it.
- High intensity focused ultrasound (HIFU) uses ultrasound waves to heat and destroy cancer cells in your prostate. HIFU is newer than some other treatments, so isn’t available everywhere and may only be available as part of a clinical trial.
- Cryotherapy uses extreme cold to freeze and destroy cancer cells. It's newer than other treatments, so isn't available everywhere and may only be available as part of a clinical trial.
Treatments aiming to control the cancer
- Hormone therapy works by either lowering the amount of testosterone in the body or by stopping it from reaching the cancer cells, wherever they are in the body. Prostate cancer cells usually need testosterone to grow.
- Radiotherapy, when combined with hormone therapy can also control prostate cancer that has spread to other parts of the body. This isn’t suitable for all men. This may include a type of external beam radiotherapy such as Stereotactic Body Radiation Therapy (SBRT).
- Chemotherapy uses anti-cancer drugs to kill cancer cells, wherever they are in the body. You may be offered chemotherapy alongside hormone therapy. It can cause some serious side effects so you will need to be fit enough to cope with these.
Some men who have recurrent prostate cancer decide to take part in clinical trials of new treatments or new combinations of existing treatments. If you are interested in taking part in a clinical trial, ask your doctor if there are any that would be suitable for you.
Monitoring your prostate cancer
You may be able to have your cancer monitored, instead of having second-line treatment straight away. For many men, prostate cancer is slow-growing and may not cause any problems or symptoms, even without treatment. The aim of monitoring is to avoid or delay treatment, and the side effects that treatment can cause.
If you decide not to have treatment straight away, your doctor and nurse will monitor you and your cancer closely for any changes. You'll have regular PSA tests. You may also have other tests and scans.
If the tests show that your cancer is growing more quickly than expected, or if you have symptoms, talk to your doctor about starting second-line treatment.
Which second-line treatments are available to me?
Several things affect which treatments are suitable, including:
- where your cancer is
- your general health
- your PSA level and other test results
- what treatment you’ve already had.
Where your cancer is
Cancer that has returned in the prostate or the prostate bed is called local recurrence. If you have local recurrence, you might be offered further treatment aiming to get rid of the cancer.
Cancer that has spread to the area just outside the prostate, but not to other parts of the body, is called locally advanced recurrence. Some men with locally advanced recurrence will also be offered treatment that aims to get rid of the cancer.
But if your cancer has spread to other parts of your body (advanced prostate cancer), then treatment can no longer cure it, but it could control the cancer for a long time. You will be offered hormone therapy and you might also be offered chemotherapy alongside it.
If your advanced prostate cancer has spread to other parts of your body but it is limited to just a few areas, this is called oligometastatic prostate cancer. If your cancer has spread to three sites or less, you might be offered a type of external beam radiotherapy called stereotactic ablative radiotherapy (SABR). This treatment can deliver high doses of radiation directly to the tumours which means it can be given in a shorter period. SABR aims to help control your cancer and delay the use of other treatments such as hormone therapy or chemotherapy.
Your general health
Your health and any other medical problems will also affect what treatments are available to you. For example, you may already have side effects from the first treatment you had. Having another treatment can cause side effects as well, so you’ll need to be fit enough to cope with this.
Your PSA level and other test results
Your PSA level and how fast it is rising will affect what treatments you are offered. You might have the option of monitoring your PSA level for a while before you have further treatment, particularly if your PSA level is rising slowly. If your PSA level is rising quickly, this suggests your cancer is more likely to have spread further.
What treatment you've already had
If your first treatment was surgery (radical prostatectomy), you might be able to have:
- radiotherapy to the prostate bed (with or without hormone therapy)
- hormone therapy alone.
If your first treatment was external beam radiotherapy, you might be able to have:
- hormone therapy
- HIFU (high-intensity focused ultrasound)
- cryotherapy
- brachytherapy
- surgery
If your first treatment was permanent seed brachytherapy or high dose-rate brachytherapy, you might be able to have:
- hormone therapy
- external beam radiotherapy
- more brachytherapy
- surgery
- cryotherapy
- HIFU, but this is rare and not available everywhere.
If your first treatment was HIFU (high-intensity focused ultrasound), you might be able to have:
- more HIFU
- external beam radiotherapy
- cryotherapy
- hormone therapy
- surgery, but this is rare.
If your first treatment was cryotherapy, you might be able to have:
- more cryotherapy
- HIFU
- external beam radiotherapy
- hormone therapy
- surgery, but this is rare
Speak to your doctor or nurse about which treatments are available to you.
Side effects of second-line treatment
All treatments have side effects. The risk of side effects is usually higher when a treatment is used as a second-line treatment than when it’s used as your first treatment. This is because your first treatment may have already caused some damage to the tissue surrounding the prostate.
Side effects may also be more severe with a second-line treatment. And you might still be getting side effects from your first treatment.
Ask your doctor or nurse for more information about the possible side effects from the second-line treatments they offer you. Read our treatment pages to find out about side effects from different treatments. Finding out about possible side effects might help you to choose between your different treatment options, or whether you want to have any treatment.
What if I don't want further treatment?
Some men weigh up the advantages and disadvantages and decide they don't want to have second-line treatment for their cancer. Speak to your doctor or nurse if you are thinking about not having further treatment. They may suggest observing your prostate cancer with regular tests. If it starts to cause symptoms then you’re likely to be offered hormone therapy to control the cancer and help relieve symptoms. There are also other treatments to manage symptoms.
When will my treatment start?
This varies from man to man. For example, your doctor might want to delay it if you are still recovering from the side effects of your first treatment. Ask your doctor or nurse for more information about when your treatment will start.
If you have treatment that aims to get rid of the cancer
If you’re having treatment that aims to get rid of the cancer, your treatment could start straight away. But for some men, there might be an option to delay treatment until tests show that the cancer is growing more quickly.
If you have treatment that aims to control your cancer
If you’re having hormone therapy to control your cancer, when you start treatment will depend on several things, including:
- whether your prostate cancer has spread to other parts of your body
- whether you have any symptoms from your cancer
- how quickly your PSA level is rising
- how you feel about starting treatment.
You might start hormone therapy straight away or you might be monitored for a while before you start. Monitoring involves regular check-ups and PSA tests. If your PSA reaches a level that suggests your cancer is growing more quickly, you will then be offered hormone therapy.
Some men feel uneasy knowing that their cancer is back and isn’t being treated, but there can be good reasons to delay hormone therapy. These include:
- if you still have side effects from your first treatment
- to delay having side effects of hormone therapy, such as sexual problems, hot flushes and fatigue.
If you are on life-long hormone therapy and having problems with side effects, you might be able to have intermittent hormone therapy.
Read more about hormone therapy and its side effects. If you are concerned about delaying the start of treatment, discuss this with your doctor or nurse.
What happens after second-line treatment?
You will have regular follow-up appointments to monitor how well your treatment is working. The aim is to:
- check how your cancer has responded to treatment
- deal with any side effects of treatment
- give you a chance to raise any concerns or ask any questions.
You will have regular PSA tests as part of this follow-up. Read more about what to expect from your follow-up care.
What if my cancer comes back again?
If your cancer comes back again after treatment that aimed to get rid of it, you will be offered hormone therapy to control your cancer, though you may not need to start it straight away.
Hormone therapy can keep your cancer under control for many months or years before you need to think about other treatments.
But over time, your cancer may start to grow again. You may continue having your original hormone therapy, but there are also other treatments available. Read more about treatment options after your first hormone therapy.
Some men decide they would like to take part in a clinical trial of a new treatment or a new combination of existing treatments.
What if I develop symptoms?
Tell your doctor or nurse about any symptoms you have. If you have symptoms between your check-ups, tell your doctor or nurse as soon as possible. If these are signs of the cancer coming back, they can talk to you about treatment options.
Your doctor or nurse can also give you advice and treatment to help manage your symptoms. For example, if your cancer has spread to the bones and is causing pain, there are treatments to help, such as pain-relieving medication, drugs called bisphosphonates and pain-relieving radiotherapy.
Dealing with recurrent prostate cancer
Some men say having prostate cancer changes the way they think and feel about life. Finding out that your prostate cancer has come back can be a particularly challenging time. You might feel scared, worried, stressed, helpless or even angry. At times, lots of men with prostate cancer get these kinds of thoughts and feelings. There’s no right way to feel and everyone reacts in their own way.
You may also have practical concerns about your cancer coming back, for example, worries about work or money.
Finding out about things you can do to help yourself can help you feel more in control. You can read more about living with or after prostate cancer and what can help. Those close to you can also find this a difficult time and they may need support and information too.
References
Updated: May 2025 | Due for review: May 2028
- Adams ES, Deivasigamani S, Mottaghi M, Huang J, Gupta RT, Polascik TJ. Evaluation of Recurrent Disease after Radiation Therapy for Patients Considering Local Salvage Therapy: Past vs. Contemporary Management. Cancers. 2023 Dec 18;15(24):5883.
- Al-Fayez S, El-Metwally A. Cigarette smoking and prostate cancer: A systematic review and meta-analysis of prospective cohort studies. Tob Induc Dis. 2023;21:19.
- Bagheri H, Mahdavi SR, Geramifar P, Neshasteh-Riz A, Sajadi Rad M, Dadgar H, et al. An Update on the Role of mpMRI and 68Ga-PSMA PET Imaging in Primary and Recurrent Prostate Cancer. Clin Genitourin Cancer. 2024 Jun;22(3):102076.
- Blank F, Meyer M, Wang H, Abbas H, Tayebi S, Hsu WW, et al. Salvage Radical Prostatectomy after Primary Focal Ablative Therapy: A Systematic Review and Meta-Analysis. Cancers. 2023 May 12;15(10):2727.
- Brookman-May SD, Campi R, Henríquez JDS, Klatte T, Langenhuijsen JF, Brausi M, et al. Latest Evidence on the Impact of Smoking, Sports, and Sexual Activity as Modifiable Lifestyle Risk Factors for Prostate Cancer Incidence, Recurrence, and Progression: A Systematic Review of the Literature by the European Association of Urology Section of Oncological Urology (ESOU). Eur Urol Focus. 2019 Sep;5(5):756–87.
- Cornford P, Tilki D, Van Den Bergh RCN, Briers E. EAU Guidelines on Prostate Cancer [Internet]. European Association of Urology; 2024 [cited 2024 May 16]. Available from: https://d56bochluxqnz.cloudfront.net/documents/full-guideline/EAU-EANM-ESTRO-ESUR-ISUP-SIOG-Guidelines-on-Prostate-Cancer-2024_2024-04-09-132035_ypmy_2024-04-16-122605_lqpk.pdf
- Darcey E, Boyle T. Tobacco smoking and survival after a prostate cancer diagnosis: A systematic review and meta-analysis. Cancer Treat Rev. 2018 Nov;70:30–40.
- Dinas PC, On Behalf Of The Students Of Module Introduction To Systematic Reviews null, Karaventza M, Liakou C, Georgakouli K, Bogdanos D, et al. Combined Effects of Physical Activity and Diet on Cancer Patients: A Systematic Review and Meta-Analysis. Nutrients. 2024 Jun 2;16(11):1749.
- Dovey Z, Horowitz A, Waingankar N. The influence of lifestyle changes (diet, exercise and stress reduction) on prostate cancer tumour biology and patient outcomes: A systematic review. BJUI Compass. 2023;4(4):385–416.
- Foerster B, Pozo C, Abufaraj M, Mari A, Kimura S, D’Andrea D, et al. Association of Smoking Status With Recurrence, Metastasis, and Mortality Among Patients With Localized Prostate Cancer Undergoing Prostatectomy or Radiotherapy: A Systematic Review and Meta-analysis. JAMA Oncol [Internet]. 2018 May 24 [cited 2018 May 29]; Available from: http://oncology.jamanetwork.com/article.aspx?doi=10.1001/jamaoncol.2018.1071
- Grubmüller B, Jahrreiss V, Brönimann S, Quhal F, Mori K, Heidenreich A, et al. Salvage Radical Prostatectomy for Radio-Recurrent Prostate Cancer: An Updated Systematic Review of Oncologic, Histopathologic and Functional Outcomes and Predictors of Good Response. Curr Oncol Tor Ont. 2021 Jul 29;28(4):2881–92.
- Hechtman LM. Clinical Naturopathic Medicine [Internet]. Harcourt Publishers Group (Australia); 2014 [cited 2015 Jul 21]. 1610 p. Available from: http://www.bookdepository.com/Clinical-Naturopathic-Medicine-Leah-Hechtman/9780729541923
- Heesterman BL, Aben KKH, de Jong IJ, Pos FJ, van der Hel OL. Radical prostatectomy versus external beam radiotherapy with androgen deprivation therapy for high-risk prostate cancer: a systematic review. BMC Cancer. 2023 May 4;23(1):398.
- Henson CC, Burden S, Davidson SE, Lal S. Nutritional interventions for reducing gastrointestinal toxicity in adults undergoing radical pelvic radiotherapy. Cochrane Database Syst Rev [Internet]. 2013 [cited 2014 Nov 18];(11). Available from: http://doi.wiley.com/10.1002/14651858.CD009896.pub2
- Houben LHP, Beelen M, van Loon LJC, Beijer S. Resistance Exercise Training, a Simple Intervention to Preserve Muscle Mass and Strength in Prostate Cancer Patients on Androgen Deprivation Therapy. Int J Sport Nutr Exerc Metab. 2024 Mar 1;34(2):122–34.
- James C, Brunckhorst O, Eymech O, Stewart R, Dasgupta P, Ahmed K. Fear of cancer recurrence and PSA anxiety in patients with prostate cancer: a systematic review. Support Care Cancer Off J Multinatl Assoc Support Care Cancer. 2022 Jul;30(7):5577–89.
- Kenfield SA, Stampfer MJ, Chan JM, Giovannucci E. Smoking and prostate cancer survival and recurrence. JAMA. 2011;305(24):2548.
- Khan S, Thakkar S, Drake B. Smoking history, intensity, and duration and risk of prostate cancer recurrence among men with prostate cancer who received definitive treatment. Ann Epidemiol. 2019 Oct 1;38:4–10.
- Kumar R, Matulewicz R, Mari A, Moschini M, Ghodoussipour S, Pradere B, et al. Impact of smoking on urologic cancers: a snapshot of current evidence. World J Urol. 2023 Jun;41(6):1473–9.
- Langlais CS, Graff RE, Van Blarigan EL, Palmer NR, Washington SL, Chan JM, et al. Post-Diagnostic Dietary and Lifestyle Factors and Prostate Cancer Recurrence, Progression, and Mortality. Curr Oncol Rep. 2021 Mar;23(3):37.
- Lavalette C, Cordina Duverger E, Artaud F, Rébillard X, Lamy PJ, Trétarre B, et al. Body mass index trajectories and prostate cancer risk: Results from the EPICAP study. Cancer Med. 2020 Sep;9(17):6421–9.
- Magnan S, Zarychanski R, Pilote L, Bernier L, Shemilt M, Vigneault E, et al. Intermittent vs Continuous Androgen Deprivation Therapy for Prostate Cancer: A Systematic Review and Meta-analysis. JAMA Oncol. 2015 Sep 17;1–10.
- Moschovas MC, Bravi CA, Dell’Oglio P, Turri F, de Groote R, Liakos N, et al. Outcomes of Salvage Robotic-assisted Radical Prostatectomy in the last decade: systematic review and perspectives of referral centers. Int Braz J Urol Off J Braz Soc Urol. 2023;49(6):677–87.
- National Institute for Clinical Excellence. High-intensity focused ultrasound for prostate cancer. Interventional procedure guidance 118. 2005.
- National Institute for Health and Care Excellence. Prostate cancer: diagnosis and management [Internet]. 2021 [cited 2022 Dec 19]. Available from: https://www.nice.org.uk/guidance/ng131
- National Institute for Health and Clinical Excellence. Cryotherapy for recurrent prostate cancer. Interventional procedure guidance 119. 2005.
- Ndjavera W, Orange ST, O’Doherty AF, Leicht AS, Rochester M, Mills R, et al. Exercise-induced attenuation of treatment side-effects in patients with newly diagnosed prostate cancer beginning androgen-deprivation therapy: a randomised controlled trial. BJU Int. 2020 Jan;125(1):28–37.
- Parker CC, James ND, Brawley CD, Clarke NW, Hoyle AP, Ali A, et al. Radiotherapy to the primary tumour for newly diagnosed, metastatic prostate cancer (STAMPEDE): a randomised controlled phase 3 trial. The Lancet. 2018 Oct;
- Peisch SF, Van Blarigan EL, Chan JM, Stampfer MJ, Kenfield SA. Prostate cancer progression and mortality: a review of diet and lifestyle factors. World J Urol. 2017 Jun;35(6):867–74.
- Pettersson A, Johansson B, Persson C, Berglund A, Turesson I. Effects of a dietary intervention on acute gastrointestinal side effects and other aspects of health-related quality of life: A randomized controlled trial in prostate cancer patients undergoing radiotherapy. Radiother Oncol. 2012 Jun;103(3):333–40.
- Purcell SA, Oliveira CLP, Mackenzie M, Robson P, Lewis JD, Prado CM. Body Composition and Prostate Cancer Risk: A Systematic Review of Observational Studies. Adv Nutr Bethesda Md. 2022 Aug 1;13(4):1118–30.
- Razdan S, Pandav K, Altschuler J, Moody K, Martin L, Patel HD, et al. Impact of exercise on continence in prostate cancer patients post robotic assisted radical prostatectomy: a systematic review. Am J Clin Exp Urol. 2023;11(4):320–7.
- Rieken M, Shariat SF, Kluth LA, Fajkovic H, Rink M, Karakiewicz PI, et al. Association of Cigarette Smoking and Smoking Cessation with Biochemical Recurrence of Prostate Cancer in Patients Treated with Radical Prostatectomy. Eur Urol. 2015 Dec;68(6):949–56.
- Sande-Rivadulla M, Alonso-Calvete A, Soto-González M. Effects of Muscle Strength Training in Prostate Cancer: A Systematic Review. Arch Esp Urol. 2024 Jan;77(1):1–15.
- Saouli A, Ruffion A, Dariane C, Barret E, Fiard G, Hankard GF, et al. Salvage Radical Prostatectomy for Recurrent Prostate Cancer: A Systematic Review (French ccAFU). Cancers. 2023 Nov 20;15(22):5485.
- Schumacher O, Luo H, Taaffe DR, Galvão DA, Tang C, Chee R, et al. Effects of Exercise During Radiation Therapy on Physical Function and Treatment-Related Side Effects in Men With Prostate Cancer: A Systematic Review and Meta-Analysis. Int J Radiat Oncol. 2021 Nov;111(3):716–31.
- Sciarra A, Santarelli V, Salciccia S, Moriconi M, Basile G, Santodirocco L, et al. How the Management of Biochemical Recurrence in Prostate Cancer Will Be Modified by the Concept of Anticipation and Incrementation of Therapy. Cancers. 2024 Feb 13;16(4):764.
- Shipley WU, Seiferheld W, Lukka HR, Major PP, Heney NM, Grignon DJ, et al. Radiation with or without Antiandrogen Therapy in Recurrent Prostate Cancer. N Engl J Med. 2017 Feb 2;376(5):417–28.
- Shore ND, Moul JW, Pienta KJ, Czernin J, King MT, Freedland SJ. Biochemical recurrence in patients with prostate cancer after primary definitive therapy: treatment based on risk stratification. Prostate Cancer Prostatic Dis. 2024 Jun;27(2):192–201.
- Spratt DE, Dess RT, Zumsteg ZS, Lin DW, Tran PT, Morgan TM, et al. A Systematic Review and Framework for the Use of Hormone Therapy with Salvage Radiation Therapy for Recurrent Prostate Cancer. Eur Urol. 2018 Feb 1;73(2):156–65.
- Steinberger E, Kollmeier M, McBride S, Novak C, Pei X, Zelefsky MJ. Cigarette smoking during external beam radiation therapy for prostate cancer is associated with an increased risk of prostate cancer-specific mortality and treatment-related toxicity. BJU Int. 2015 Oct;116(4):596–603.
- Stewart RJ, Humphris GM, Donaldson J, Cruickshank S. Does Cancer Type Influence the Impact of Recurrence? A Review of the Experience of Patients With Breast or Prostate Cancer Recurrence. Front Psychol. 2021;12:635660.
- Tillisch K. Complementary and alternative medicine for functional gastrointestinal disorders. Gut. 2006 May 1;55(5):593–6.
- Vale CL, Fisher DJ, Godolphin PJ, Rydzewska LH, Boher JM, Burdett S, et al. Which patients with metastatic hormone-sensitive prostate cancer benefit from docetaxel: a systematic review and meta-analysis of individual participant data from randomised trials. Lancet Oncol. 2023 Jul;24(7):783–97.
- Valle LF, Lehrer EJ, Markovic D, Elashoff D, Levin-Epstein R, Karnes RJ, et al. A Systematic Review and Meta-analysis of Local Salvage Therapies After Radiotherapy for Prostate Cancer (MASTER). Eur Urol. 2021 Sep;80(3):280–92.
- Van den Broeck T, van den Bergh RCN, Arfi N, Gross T, Moris L, Briers E, et al. Prognostic Value of Biochemical Recurrence Following Treatment with Curative Intent for Prostate Cancer: A Systematic Review. Eur Urol [Internet]. 2018 Oct [cited 2019 Feb 22]; Available from: https://linkinghub.elsevier.com/retrieve/pii/S0302283818307528
- Vyas N, Brunckhorst O, Fanshawe JB, Stewart R, Dasgupta P, Ahmed K. Prognostic factors for mental wellbeing in prostate cancer: A systematic review and meta-analysis. Psychooncology. 2023;32(11):1644–59.
- Walz S, Maas M, Stenzl A, Todenhöfer T. Bone Health Issues in Patients with Prostate Cancer: An Evidence-Based Review. World J Mens Health. 2020 Apr;38(2):151–63.
- Wedlake LJ, Shaw C, Whelan K, Andreyev HJN. Systematic review: the efficacy of nutritional interventions to counteract acute gastrointestinal toxicity during therapeutic pelvic radiotherapy. Aliment Pharmacol Ther. 2013 Jun;37(11):1046–56.
- Wolin KY, Luly J, Sutcliffe S, Andriole GL, Kibel AS. Risk of Urinary Incontinence Following Prostatectomy: The Role of Physical Activity and Obesity. J Urol. 2010 Feb;183(2):629–33.
- World Cancer Research Fund International. Continuous Update Project report: Diet, Nutrition, Physical Activity and Prostate Cancer [Internet]. 2014. Available from: https://www.wcrf.org/wp-content/uploads/2021/02/prostate-cancer-report.pdf
- Wullaert L, Voigt KR, Verhoef C, Husson O, Grünhagen DJ. Oncological surgery follow-up and quality of life: meta-analysis. Br J Surg. 2023 May 16;110(6):655–65.
- Yuan F, Wang Y, Xiao X, Zhang X, Jing M, Kamecki H, et al. A systematic review evaluating the effectiveness of exercise training on physical condition in prostate cancer patients undergoing androgen deprivation therapy. Transl Androl Urol. 2023 Aug 31;12(8):1336–50.

